What is IBS? And do I have it?
01/11/18We bring you nutrition information that you can trust – all our articles are researched and evidence based.
What is IBS?
IBS is a chronic and fluctuating condition with a variety of symptoms including bloating, wind, abdominal pain, diarrhoea and or constipation. Some patients also experience nausea, lethargy, stomach grumbling and reflux (1,2). Symptoms can fluctuate in severity and people frequently experience ‘flare ups’. It is often a lifelong condition but can be managed through diet and lifestyle advice. It can severely affect people’s quality of life and work productivity (1).

What causes IBS?
There is no known definitive cause of IBS but current research suggests possible causes are (1,2,3):
- Altered gut motility – either slow or fast gut transit
- After an attack of gastroenteritis – can alter gut microbiome and trigger IBS type symptoms
- Immune activation
- Small intestinal bacterial overgrowth
- Visceral hypersensitivity – a lower pain threshold within the GI tract
- Use of powerful antibiotics – can alter the gut microbiome and trigger symptoms
- Psychological trauma or stress
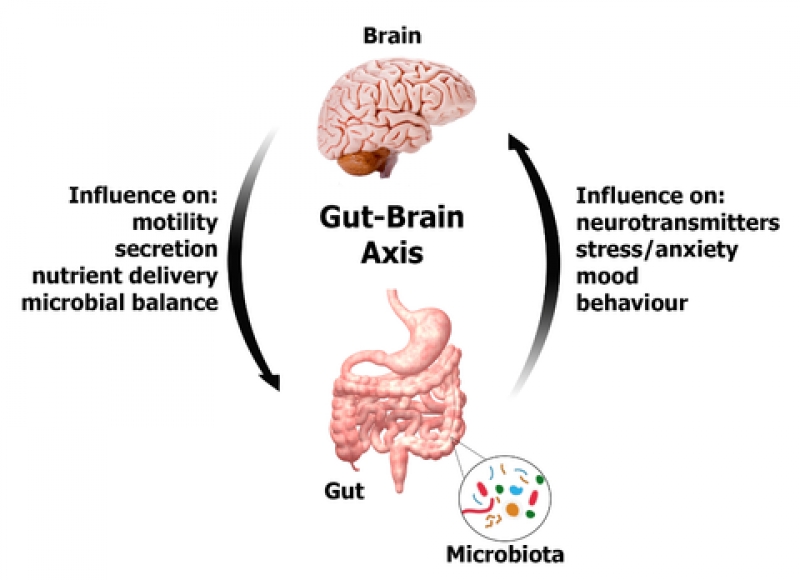
- Gut-brain axis – our central nervous system can affect physiological response
Whatever the possible cause, there are also known triggers which can make the condition worse such as diet, stress, medications and lack of physical activity.
How can you be sure you have IBS?
The symptoms described above can also be attributed to other conditions such as inflammatory bowel disease, coeliac disease, food allergy, small intestinal bacterial overgrowth, malignancy, gallbladder issues and pancreatitis to name but a few.
There is no direct biomarker test to determine if you have IBS but rather tests are taken to rule out these other conditions. Never assume you just have IBS so it is important if you have gastroenterology symptoms that you start with a visit to your GP; he will undertake a series of routine blood and stool tests to rule out inflammatory bowel disease, coeliac disease etc. as well as a physical exam (3, 6).
It is also important that if you have any of the following symptoms that you go to your GP straightaway (6):
- Unexplained weight loss
- Passing blood in your stools
- Any lumps or swelling in the abdomen
- If you are over 50 and have recently developed altered bowel function
- Family history of bowel or ovarian cancer
If all your initial tests are negative and your GP feels certain it is IBS, then it is a good time to look at diet and lifestyle factors to help manage your condition. Sometimes your GP may send you to a gastroenterology consultant for further tests.
I’ve been diagnosed with IBS – now what?
Once diagnosed with IBS, people are often left to manage the condition themselves. Unfortunately, there is a lot of misleading information available online which can become confusing. Further, there is no one single identifiable factor that works for everyone – everyone’s gut is different and is sensitive to its own particular triggers. It takes time and the right support to improve gut function. The main areas to look at are:
Diet
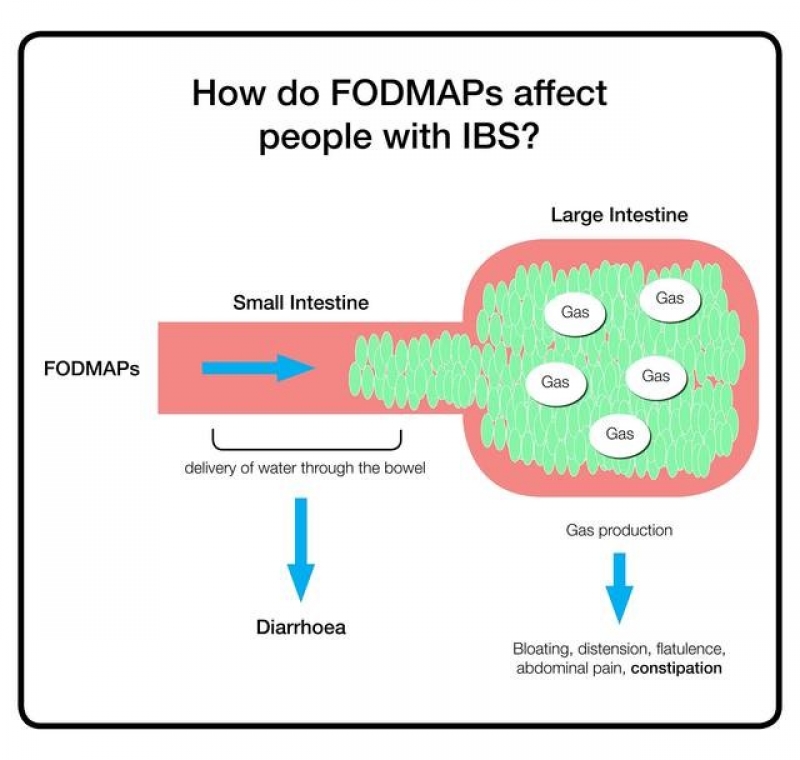
Diet can have a significant impact on gut function. Over recent years, the FODMAP diet has been clinically proven to improve IBS symptoms in up to 70% of patients (5, 6). This diet focuses on the types of fermentable fibres in your diet which can increase gas production and cause wind, bloating, diarrhoea. The diet involves a temporary reduction in fermentable fibres to achieve symptom relief and then is followed by a reintroduction phase with one food being introduced at a time to identify your particular food trigger. Whilst there are several versions of FODMAP available on the internet, to give yourself the best chance of success it is important to undertake the FODMAP diet with a dietitian who is trained in this and will guide you through it step by step; this makes following the diet much easier and ensures nutritional adequacy.
Other dietary factors can be due to food allergies such as wheat or dairy proteins. Further, people can be sensitive to other known gut irritants such as chilli, alcohol, caffeine.
Again, working with a skilled clinical dietitian, you will be guided through assessment and dietary changes systematically to identify your triggers, safely.
Probiotics
The research in the effectiveness of probiotics and IBS is growing with a trend towards positive results, however the evidence remains limited on the use of probiotic strains and quantities (6). Certain probiotics can improve some IBS symptoms for some patients but may not be effective for all patients. Check with your dietitian whether probiotics are indicated and for advice on probiotic strains most appropriate for your symptoms.

Stress
Times of acute stress are known to affect gut function as are chronic or low levels of ongoing anxiety/stress. People with anxiety disorders are also known to have a higher incidence of IBS symptoms (3).
If you feel stress is contributing to your symptoms then is it worthwhile looking at ways to reduce this stress. There are various options and the key is to find the right treatment to suit you, for example, cognitive behavioural therapy, symptom directed hypnotherapy and mindfulness based therapy have all been shown to be helpful in improving IBS symptoms (8).
Exercise
Even a moderate increase in physical activity can stimulate gut muscles and improve bowel function. It also has the added benefit of being able to improve relaxation and decrease stress and anxiety (6). Talk with your health professional if you are unsure about the way to increase your activity and the right activity for you.
Summary
IBS is a chronic and often relapsing condition with no known obvious cause but there are identified triggers such as diet and stress.
Symptoms can include wind, bloating, abdominal pain and cramps, diarrhoea and/or constipation, nausea, reflux and stomach grumbling. It can have significant impact on quality of life.
It is important to make sure that your symptoms are due to IBS and not another cause so always check with your GP as a starting point.
If you have been diagnosed with IBS then there are positive steps you can do with diet, lifestyle and probiotics to help you improve and manage your condition.
The complexity and diversity of IBS presentation can make it a challenging process to self-manage so always seek professional support when undertaking dietary changes with a qualified dietitian.
Jeanette Starkey
Specialist Gastroenterology Dietitian
Vie Nutrition, Dietetic Consultancy
1 November 2018
References
- Chey, W.D., Kurlander, J. and and Eswaran, S. (2015) Irritable bowel syndrome. A clinical review. JAMA. 313(9), 949-958
- Drossman, D.A. (2016) Functional gastrointestinal disorders: history, pathophysiology, clinical features, and Rome IV.Gastroenterology. 150, 1262-1279
- L. Saha. (2014). Irritable bowel syndrome: Pathogenesis, diagnosis, treatment, and evidence-based medicine; World J Gastroenterol; 20(22): 6759–6773
- Lee, C. et al (2017). The Increased Level of Depression and Anxiety in Irritable Bowel Syndrome Patients Compared with Healthy Controls: Systematic Review and Meta-analysis. J Neurogastroenterol Motil; Jul 30; 23(3):349-362
- McKenzie, Y.A., Bowyer, R.K. and Leach, H. et al (2016) British Dietetic Association systematic review and evidence-based practice guidelines for the dietary management of irritable bowel syndrome in adults (2016 update). Journal of Human Nutrition and Dietetics. 29(5), 549-575.
- Nice Guidelines (2017): Irritable bowel syndrome in adults: diagnosis and management;
- McKenzie, Y.A. et al. (2016). British Dietetic Association systematic review of systematic reviews and evidence-based practice guidelines for the use of probiotics in the management of irritable bowel syndrome in adults J Hum Nutr Diet; 29(5):576-92
- Ballou, S and Keefer, L. (2017). Psychological Interventions for Irritable Bowel Syndrome and Inflammatory Bowel Diseases Clin Transl Gastroenterol; 8(1): e214
Latest posts
Welcome to Vie Nutrition Dietetic Consultancy
27/08/18Welcome to our first blog post from Vie Nutrition. We are a dietetic consultancy based in Chester... Read more...


 07810 633 789
07810 633 789 